Prostatitisis an inflammatory disease of the prostate. It is manifested by frequent urination, pain in the penis, scrotum, rectum, sexual disorders (erection disorder, early ejaculation, etc. ), sometimes urinary retention, blood in the urine. The diagnosis of prostatitis is made by a urologist or an andrologist according to the typical clinical picture and the results of a rectal examination. In addition, an ultrasound of the prostate, bakposev of the prostate and urine is performed. Treatment is conservative - antibiotic therapy, immunotherapy, prostate massage, lifestyle correction.

General information
Prostatitis is an inflammation of the seminal (prostate) gland - the prostate. It is the most common disease of the genitourinary system in men. It most often affects patients aged 25-50. According to various data, 30-85% of men over the age of 30 suffer from prostatitis. Possible formation of prostate abscess, inflammation of the testicles and appendages, which threatens infertility. The rise of infection leads to inflammation of the upper genitourinary system (cystitis, pyelonephritis).
The pathology develops through the penetration of an infectious agent that enters the prostate tissue from the organs of the genitourinary system (urethra, bladder) or from a distant focus of inflammation (with pneumonia, flu, tonsillitis, furunculosis).
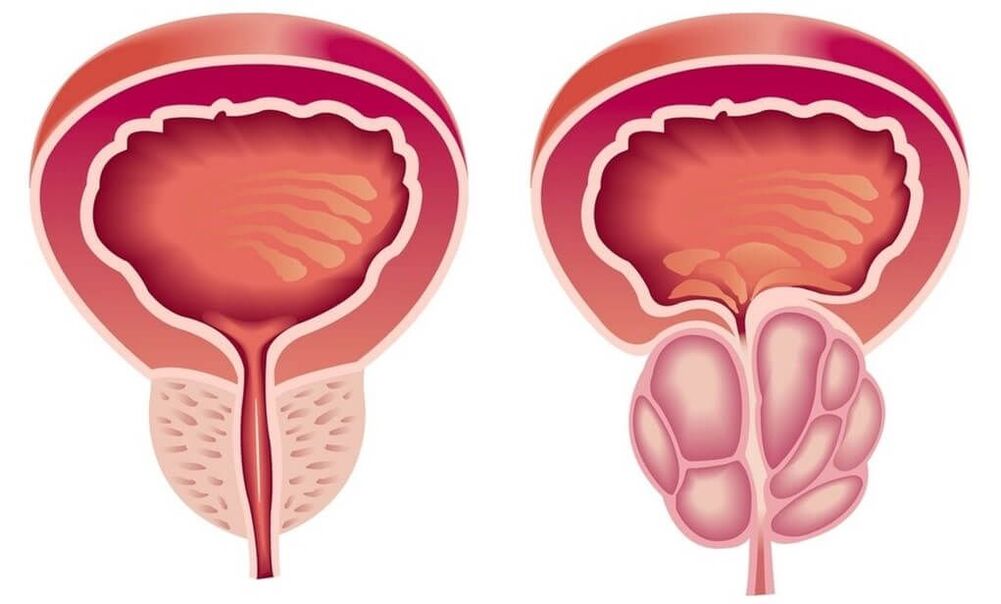
Causes of prostatitis
Staphylococcus aureus (Staphylococcus aureus), Enterococcus (Enterococcus), Enterobacter (Enterobacter), Pseudomonas (Pseudomonas), Proteus (Proteus), Klebsiella (Klebsiella) and Escherichia coli can act as an infectious agent in the acute process. . Most microorganisms belong to conditionally pathogenic flora and cause prostatitis only in the presence of other predisposing factors. Chronic inflammation is usually the result of polymicrobial associations.
The risk of developing the disease increases with hypothermia, a history of specific infections and conditions accompanied by congestion in the prostate tissues. There are the following predisposing factors:
- General hypothermia (single or permanent, related to working conditions).
- Sedentary lifestyle, a specialty that forces a person to be in a sitting position for a long time (computer operator, driver, etc. ).
- Constant constipation.
- Violations of the normal rhythm of sexual activity (excessive sexual activity, prolonged abstinence, incomplete ejaculation during "usual" sexual intercourse devoid of emotional color).
- The presence of chronic diseases (cholecystitis, bronchitis) or chronic infectious foci in the body (chronic osteomyelitis, untreated caries, tonsillitis, etc. ).
- Previous urological diseases (urethritis, cystitis, etc. ) and sexually transmitted diseases (chlamydia, trichomoniasis, gonorrhea).
- Conditions that cause suppression of the immune system (chronic stress, irregular and malnutrition, regular lack of sleep, overtraining of athletes).
It is assumed that the risk of developing pathology increases with chronic intoxication (alcohol, nicotine, morphine). Some research in the field of modern andrology proves that chronic perineal trauma (vibration, concussion) in drivers, motorcyclists and cyclists is a provoking factor. However, the vast majority of experts believe that all these circumstances are not the real causes of the disease, but only contribute to the worsening of the latent inflammatory process in the prostate tissues.
Congestion in prostate tissues plays a decisive role in the development of prostatitis. Violation of capillary blood flow causes an increase in lipid peroxidation, edema, excretion of prostate tissue and creates conditions for the development of an infectious process.
Symptoms of prostatitis
Acute prostatitis
There are three stages of acute prostatitis, characterized by the presence of a certain clinical picture and morphological changes:
- Acute catarrhal. Patients complain of frequent, often painful urination, pain in the sacrum and perineum.
- Acute follicular. The pain becomes more intense, sometimes spreads to the anus, aggravated by defecation. Urination is difficult, urine flows in a thin stream. In some cases, urine retention occurs. A subfebrile state or moderate hyperthermia is typical.
- Acute parenchyma. Severe general intoxication, hyperthermia up to 38-40°C, chills. Dysuric disorders, often - acute retention of urine. Sharp, throbbing pains in the perineum. Difficulty in defecation.
Chronic prostatitis
In rare cases, chronic prostatitis becomes the result of an acute process, however, as a rule, a primary chronic course is observed. The temperature occasionally rises to subfebrile values. The patient notices slight pain in the perineum, discomfort during urination and defecation. The most characteristic symptom is scanty discharge from the urethra during defecation. The primary chronic form of the disease develops over a long period of time. It is preceded by prostatosis (stagnation of blood in the capillaries), which gradually turns into abacterial prostatitis.
Chronic prostatitis is often a complication of the inflammatory process caused by the causative agent of a certain infection (chlamydia, trichomonas, ureaplasma, gonococcus). Symptoms of a specific inflammatory process in many cases mask the manifestations of prostate damage. Perhaps a slight increase in pain during urination, slight pain in the perineum, scanty discharge from the urethra during defecation. A slight change in the clinical picture often goes unnoticed by the patient.
Chronic inflammation of the prostate can be manifested by a burning sensation in the urethra and perineum, dysuria, sexual disorders, increased general fatigue. Mental depression, anxiety and irritability are often the result of impairment of potency (or fear of these impairments). The clinical picture does not always include all the listed groups of symptoms, it differs in different patients and changes over time. There are three main syndromes characteristic of chronic prostatitis: pain, dysuric, sexual disorders.
There are no pain receptors in prostate tissue. The cause of pain in chronic prostatitis becomes almost inevitable due to abundant innervation of the pelvic organs, involvement in the inflammatory process of nerve pathways. Patients complain of pain of varying intensity - from weak, painful to intense, disturbing sleep. There is a change in the nature of pain (increasing or weakening) during ejaculation, excessive sexual activity or sexual abstinence. The pain spreads to the scrotum, sacrum, perineum, sometimes to the lumbar region.
As a result of inflammation in chronic prostatitis, the volume of the prostate increases, squeezing the urethra. The lumen of the ureter is reduced. The patient has a frequent need to urinate, a feeling of incomplete emptying of the bladder. As a rule, dysuric phenomena are expressed in the early stages. Compensatory hypertrophy of the muscle layer of the bladder and ureter then develops. Symptoms of dysuria during this period weaken, and then increase again with the decompensation of adaptive mechanisms.
In the initial stages, dyspotency can develop, which manifests itself differently in different patients. Patients may complain of frequent nocturnal erections, blurred orgasm or worsening erection. Accelerated ejaculation is associated with a decrease in the threshold level of orgasmic center excitation. Painful sensations during ejaculation can cause rejection of sexual activity. In the future, sexual dysfunctions become more pronounced. In the advanced stage, impotence develops.
The degree of sexual disorder is determined by many factors, including the sexual constitution and psychological state of the patient. Potency disorders and dysuria can be caused both by changes in the prostate and by the suggestibility of the patient, who, if he has chronic prostatitis, expects the inevitable development of sexual disorders and urination disorders. Especially often, psychogenic dyspotency and dysuria develop in suggestible, anxious patients.
Impotence, and sometimes the very danger of possible sexual disorders, is hard for patients to bear. Often there is a change in character, irritability, discomfort, excessive concern for one's own health, and even "worry about illness".
Complications
In the absence of timely treatment of acute prostatitis, there is a significant risk of developing a prostate abscess. With the formation of a purulent focus, the patient's body temperature rises to 39-40 ° C and can become hectic. Periods of heat alternate with severe cold. Sharp pains in the perineum make it difficult to urinate and prevent defecation.
An increase in prostate edema leads to acute retention of urine. Rarely, an abscess spontaneously ruptures in the urethra or rectum. When it opens, purulent, cloudy urine with an unpleasant pungent odor appears in the urethra; when opened, the stool contains pus and mucus in the rectum.
Chronic prostatitis is characterized by an undulating course with periods of long-term remissions, during which the inflammation in the prostate is latent or manifests itself with extremely bad symptoms. Patients who don't mind often stop treatment and only turn around when complications develop.
The spread of infection through the urinary tract causes pyelonephritis and cystitis. The most common complication of the chronic process is inflammation of the testicles and epididymis (epdidymo-orchitis) and inflammation of the seminal vesicles (vesiculitis). The outcome of these diseases is often infertility.
Diagnostics
A characteristic clinical picture simplifies the process of diagnosis in acute and chronic prostatitis. It is mandatory:
Treatment of prostatitis
Treatment of acute prostatitis
Patients with an uncomplicated acute process are treated by a urologist on an outpatient basis. In case of severe intoxication, suspected purulent process, hospitalization is indicated. Antibacterial therapy is administered. Preparations are chosen taking into account the sensitivity of the infectious agent. Antibiotics are widely used and can penetrate well into the tissues of the prostate.
With the development of acute retention of urine on the background of prostatitis, they resort to the installation of a cystostomy rather than a urethral catheter, because there is a risk of prostate abscess formation. With the development of an abscess, endoscopic transrectal or transurethral opening of the abscess is performed.
Treatment of chronic prostatitis
Treatment of chronic prostatitis should be complex, including etiotropic therapy, physiotherapy, correction of immunity:
- Antibiotic therapy. The patient is prescribed long courses of antibacterial drugs (within 4-8 weeks). The selection of the type and dose of antibacterial drugs, as well as the determination of the duration of the course of treatment, is carried out individually. The drug is selected based on the sensitivity of the microflora according to the results of urine culture and prostate secretion.
- Prostate massage.Massage of the gland has a complex effect on the affected organ. During the massage, the inflammatory secret accumulated in the prostate is squeezed into the channels, then enters the urethra and is removed from the body. The procedure improves blood circulation in the prostate, which minimizes clogging and ensures better penetration of antibacterial drugs into the tissue of the affected organ.
- Physiotherapy.Laser exposure, ultrasound waves and electromagnetic vibrations are used to improve blood circulation. If it is impossible to carry out physiotherapeutic procedures, the patient is prescribed warm medicinal microclysters.
In the case of chronic, long-term inflammation, a consultation with an immunologist is indicated for the selection of immunocorrective therapy tactics. The patient is given advice on lifestyle changes. Certain changes in the lifestyle of patients with chronic prostatitis are both curative and preventive. Normalization of sleep and wakefulness, establishment of diet, moderate physical activity are recommended to the patient.
Antibiotic therapy is the most effective treatment for prostatitis. Phytotherapy, immunocorrectors and hormonal preparations can also be used according to the doctor's recommendation.
In the absence of acute symptoms, prostatitis can be treated with physiotherapy methods. In case of abscesses and suppurations, surgical intervention is recommended.
Drug treatment
The treatment of prostatitis with antibiotic therapy should begin with a swab, the purpose of which is to assess the sensitivity of the organism to this type of antibiotic. In violation of urination, a good result is the use of anti-inflammatory drugs.
Medicines are taken in tablets, in acute cases - in the form of a dropper or intramuscularly. Rectal suppositories are effective for the treatment of chronic forms of prostatitis: with their help, drugs reach their goal faster and have a minimal effect on other organs.
Blood thinners and anti-inflammatory drugs have also worked well.
Antibacterial therapy
Antibiotics are an effective drug in the fight against bacterial prostatitis. In order to achieve the desired effect and not damage the body, the choice of medicine, dosage and treatment regimen should be handled by a doctor. For the correct selection of the most effective drugs, it will be necessary to find out which type of pathogen caused prostatitis, and also check the patient's tolerance to antibiotics of a certain group.
Antibiotics from the fluoroquinolone group have been well proven for effective treatment of chronic prostatitis. Their action is aimed at suppressing bacterial infection and strengthening one's own immunity. In addition, a bacteriostatic antibiotic is recommended for the prevention and treatment of concomitant diseases of the genitourinary system.
Treatment of prostatitis caused by mycoplasma and chlamydia can be additionally carried out with macrolide and tetracycline drugs that slow down the spread of the infection.
The duration of taking antibacterial drugs is from 2 to 4 weeks. In case of positive dynamics, the course can be extended.
Physiotherapy
Physiotherapy methods in the treatment of prostatitis are aimed at activating blood circulation in the pelvic area, improving metabolic processes in the prostate and cleaning the ducts. If physiotherapy is combined with taking antibiotics, then the effect of the latter is enhanced.
The main methods include:
- magnetotherapy;
- laser therapy;
- electrophoresis;
- warming up;
- ultrasound;
- mud treatment;
- high frequency radiation;
- physiotherapy.
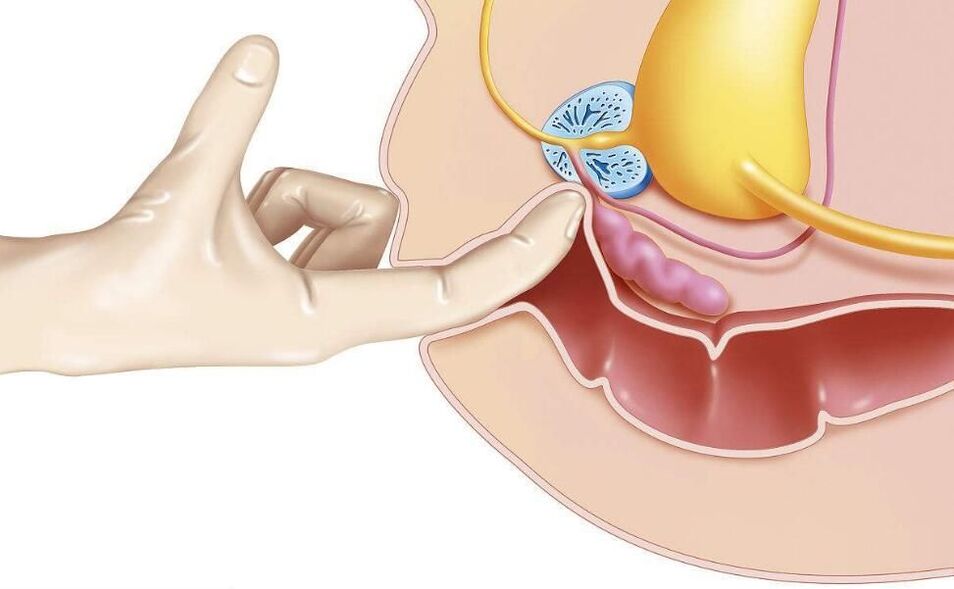
One of the oldest methods - transrectal massage of the prostate, according to modern research, has no proven effectiveness.
Non-specific treatments
Non-specific treatments for prostatitis include:
- hirudotherapy;
- medicinal fasting;
- acupuncture;
- diet according to Ostrovsky's method;
- alkalization of the body according to the Neumyvakin method.
All non-traditional methods of prostatitis treatment are strongly recommended to be agreed with your doctor.
Operation
Surgical methods are used in complex and urgent cases:
- for drainage of purulent abscesses, which are removed by laparoscopic methods through puncture;
- in violation of urination due to damage to the urinary tract;
- with a large volume of the affected area;
- with a significant number of stones in the body of the gland.
Stones and sclerosed tissues are removed by endoscopic methods. In the case of a large area of damage or multiple stones, resection of the prostate is resorted to.
Transurethral resection is also effective in bacterial prostatitis. Thus, it is possible to reduce the risk of relapse.
Folk remedies
Treatment of prostatitis with folk remedies is unlikely to be effective by itself, but in combination with medical and physiotherapeutic methods it may be applicable. These include: beekeeping products, decoctions of herbs and seeds, tinctures of garlic, ginger, beaver creek, fresh vegetables, pumpkin seeds.
In acute cases of the course of the disease, it is necessary to consult a doctor, and in no case should you self-medicate! In the case of rupture of a purulent abscess, a fatal outcome is possible.
Candles for prostatitis
Treatment of prostatitis with rectal suppositories is much more effective than pills, if only because the rectum is much closer to the prostate, which means that the medicine will work faster.
The composition of drugs for the treatment of prostatitis can be completely different, they are prescribed to solve a specific problem.
- Antibacterial agents are particularly effective in prostatitis caused by chlamydia.
- Painkillers are used for symptomatic treatment, they relieve pain well.
- Immunostimulants improve blood circulation, relieve swelling and are used in complex therapy.
- Phytopreparations have a mild effect. They, like candles on bee products, are used as an addition to the main treatment.
- Compositions based on ichthyol promote blood flow in the area of the intestinal mucosa, which accelerates the weakening of inflammatory processes and slightly improves immunity.
- Enzyme-based products prevent the formation of scar tissue. It is recommended to be taken as part of complex therapy with antibiotics, anti-inflammatory and analgesic drugs.
Auxiliary drugs
For the symptomatic treatment of prostatitis in men, such as relieving pain when urinating, you can additionally take antispasmodics that relax smooth muscles and thus quickly relieve pain.
Dietary supplements for blood thinning and anti-inflammatory based on bee products, pumpkin oil, palm fruit extract contribute to general recovery.
Diet and lifestyle
A proper, balanced diet and a healthy lifestyle are very important for the treatment of prostatitis. Food should not contain spicy, fried, salty, sour food. In acute form, alcohol is strictly prohibited.
Food should contain enough fiber to prevent constipation. The protein content should be reduced. It is advisable to supplement the diet with herbs, ginger, and pumpkin seeds.
Treatment without drugs
Medicine-free therapy methods allow you to act directly on the prostate, increase the concentration of drugs in its tissues, and help remove congestion.
Microwave hyperthermia is performed using a rectal probe that is inserted into the patient's anus. On the device, you can set the temperature required for a certain type of exposure. To increase the concentration of the drug in the prostate, it is necessary to heat it to 38-40°C. To achieve an antibacterial effect - 40-45 °C.
Today, non-drug therapy focuses on laser therapy. The possibilities of this technique are wide. Under the influence of the laser in the prostate, the following processes occur:
- activation of redox reactions;
- improves blood microcirculation;
- new capillaries are formed;
- pathogenic microflora is suppressed;
- the process of cell division is activated, which contributes to tissue regeneration.
During the research period of the effects of laser therapy on patients with prostatitis, a side effect was observed, but positive for treatment purposes. In those who completed the course, potency increased, erectile dysfunction was eliminated, and vitality was restored. To achieve this result, it is necessary to use a beam of a certain wavelength. In general, low-intensity laser radiation is used to treat chronic prostatitis.
Patients can undergo laser therapy on their own initiative, if not prescribed by the attending physician.
Surgical treatment of chronic prostatitis
Chronic prostatitis does not pose a threat to the patient's life, but it can significantly reduce its quality. The most serious complication of this disease is the formation of stones in the gland tissues. Transurethral resection is used to get rid of protoliths.
The operation is performed under the control of TRUS.
If complications such as prostate sclerosis occur, transurethral electrosurgery is performed. If sclerosis of the bladder neck is observed in combination with this pathology, a partial resection of the prostate is performed.
With the blockage of the seminal and excretory ducts, endoscopic operations are indicated to remove violations of the patency of the secret. For this purpose, an incision is made in the seminal vesicles and ducts. In the case of an abscess, it is possible to completely remove the gland.
Consequences of untreated prostatitis

Even if the symptoms of prostatitis do not appear for a long time, it is necessary to undergo a regular examination by a urologist. Incompletely cured prostatitis can be accompanied by the formation of calcifications, which must then be removed together with the gland. Experts are sure that there are no other ways to remove or dissolve limescale.
In addition, pathogenic microorganisms can migrate to neighboring organs, causing inflammation. Flowing prostatitis can cause the development of prostate adenoma and cancer.
Prognosis and prevention
Acute prostatitis is a disease that has a pronounced tendency to become chronic. Even with timely and adequate treatment, more than half of patients end up with chronic prostatitis. Recovery is far from always achieved, however, with proper consistent therapy and adherence to the doctor's recommendations, it is possible to eliminate unpleasant symptoms and achieve long-term stable remission in a chronic process.
Prevention is the removal of risk factors. It is necessary to avoid hypothermia, alternating sedentary work and periods of physical activity, eating regularly and fully. Laxatives should be used for constipation. One of the preventive measures is the normalization of sexual life, because both excessive sexual activity and sexual abstinence are risk factors for the development of prostatitis. If symptoms of a urological or sexually transmitted disease appear, it is necessary to consult a doctor in a timely manner.





























